17 February 2011
Clean water and education could outperform vaccines at reducing Haiti cholera epidemic
Posted by Michael McFadden
Guest post by Liz Borkowski, Research Associate at the George Washington University School of Public Health’s Department of Environmental and Occupational Health. Liz has blogged about the Haiti cholera outbreak from a public health perspective on her blog The Pump Handle.
Even though the deadly cholera epidemic in Haiti is now spreading more slowly, health officials are still working to prevent as many new cases as possible. Detailed models of the disease’s spread help those in charge of making public health decisions understand the effectiveness of control measures, from vaccines to investments in clean water supply and education.
A new study by Enrico Bertuzzo and colleagues just accepted for publication in Geophysical Research Letters looks at how the Haitian cholera outbreak is likely to evolve and finds that, now that the disease is a nationwide epidemic, clean water and hygiene education measures are likely to be more effective at reducing cholera’s residual progression in the country than a vaccination campaign.
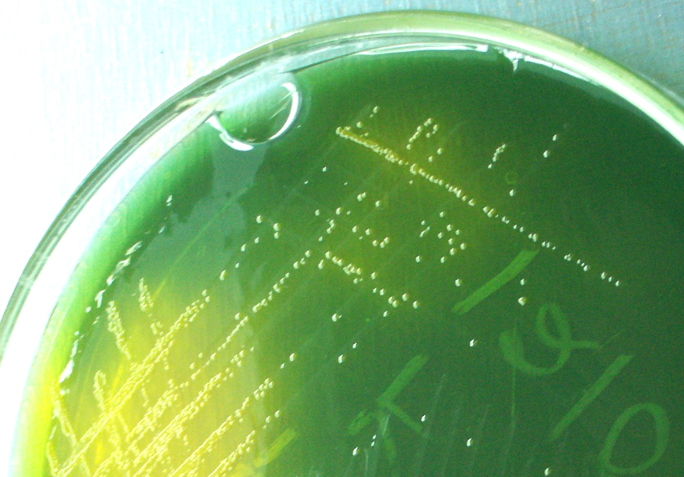
Cholera bacteria (Vibrio cholerae) spread mainly through fecal contamination of water, and the study describes the two main mechanisms of that spread: hydrologic pathways (because the bacteria can survive and travel through aquatic environments) and travel by infected people (who may or may not exhibit symptoms). The researchers used a dispersion model and information about more than 500 Haitian communities to predict the spread of V. cholerae and the cholera cases that would result.
Based on their modeling (which the researchers carried out before mid January), the team predicted that new cases would start decreasing in January, and that is in fact what happened. In late January, Haiti’s health ministry reported that new cases had dropped to about 4,700 per week (a substantial decline since November, when 12,000+ new cases were reported each week). By then, cholera had killed nearly 4,000 people and sickened more than 194,000.
Bertuzzo’s team modeled the effect of a campaign to vaccinate 150,000 people (the maximum possible given the vaccine supply) in Port-au-Prince starting on January 1, 2011 and discovered the benefits would have been negligible. They note that this intervention’s small effectiveness is due partly to the slow pace at which full immunity builds up and to the likelihood that many vaccine recipients would’ve already built up natural immunity through asymptomatic infections.
By contrast, results suggest that clean water and hygiene education measures could be much more effective at reducing cholera’s residual progression in Haiti. The modeling assumed that these prevention measures would reduce the probability of ingesting contaminated water or food during a one-month timespan by 40%, and the authors note that the feasibility of achieving this under Haiti’s current conditions is debatable. Still, it’s useful for health officials to know what kind of target an intervention will need to achieve in order to reduce cholera’s progress. Then, they can focus on finding and deploying the resources necessary to make the intervention effective.
![]()
E. Bertuzzo, L. Mari, L. Righetto, M. Gatto, R. Casagrandi, M. Blokesch, I. Rodriguez-Iturbe, & A. Rinaldo (2011). Prediction of the spatial evolution and effects of control measures for the unfolding Haiti cholera outbreak Geophysical Research Letters : 10.1029
— Liz Borkowski, Research Associate at the George Washington University School of Public Health










 GeoSpace is a blog on Earth and space science, managed by AGU’s Public Information staff. The blog features posts by AGU writers and guest contributors on all sorts of relevant science topics, but with a focus on new research and geo and space sciences-related stories that are currently in the news.
GeoSpace is a blog on Earth and space science, managed by AGU’s Public Information staff. The blog features posts by AGU writers and guest contributors on all sorts of relevant science topics, but with a focus on new research and geo and space sciences-related stories that are currently in the news.
[…] This post was mentioned on Twitter by Am Geophysical Union, greatcircle. greatcircle said: RT @theAGU: Clean water and education could outperform vaccines at reducing #Haiti cholera epidemic http://bit.ly/eBMPIk [Guest GeoSpace … […]
[…] American Geophysical Union February 17, 2011 Full article here: […]
Hi, I’m a student currently researching cholera and the effects of the vaccine and clean water. And I was wondering if there was any data ( could be any graphs or number stats) for the report that could be shown, for the report above.
Kind regards